The anatomy of polyvagal structures
- Tjasa Cerovsek Landes LMT
- Dec 3, 2019
- 6 min read
Updated: Dec 17, 2025

It was last year that I dove deep into studying about Dr. Steven Porges' Polyvagal Theory. As a manual therapist and bodyworker I found many aspects of the theory relevant to me. Perhaps I will elaborate on what the Theory is another time, or you may have already heard about it. Today I want to share with you my sketches that helped me understand the anatomy of the vagus nerves and also how the poly-vagal theory translates into anatomy.
A quick run down of the Autonomic Nervous System (ANS) first. The ANS is that part of our nervous system that is automatic and autonomic. It regulates digestion, breathing, heart rate, sleep, all of those things we rely on 24/7 but never need to give it a thought. It does so many things and this blog is not intending to go down that lane. However, according to the Polyvagal Theory (PVT) we now understand that our social engagement is also regulated by the Autonomic Nervous System, of which vagus nerve is a big part.
The Autonomic Nervous System has two branches: the Parasympathetic and the Sympathetic branch. But you know that already, so I'll jump to the Vagus nerve. Although we read about the Vagus nerve as if there is one singular nerve, it is a paired cranial nerve (no. 10, or CN X). We have a left and a right Vagus nerve branches. FYI Some fish (like goldfish) don't have vagal nerves, but possess a vagal lobe instead, which among other crucial functions helps them sort food from stones :)
As 'polyvagal' suggests that there isn't one vagal nerve, but many - poly. Left and right, as well as Dorsal and Ventral vagal complexes, which really translate into myelinated and unmyelinated Vagus nerves. We can also divide the Vagus nerves into supra diaphragmatic and sub diaphragmatic.
As per PVT, the differentiation between myelinated and unmyelinated fibers of the vagus nerve goes beyond the myelin division. The differentiation and consequent naming of each implies that unmyelinated fibers are phylogenetically older and associated with survival in unsafe environment, whereas myelinated fibers evolved much later and serve mammalian species exclusively and are associated with function within safe environment. Unmyelinated fibers belong to the Dorsal Vagal Complex, and myelinated fibers to the Ventral Vagal Complex.
Keep on reading, here comes a picture of that...
THE VAGUS NERVE DISSECTION
Let's take a single Vagus nerve and look inside.

Anatomists largely agree that between 75%-85% of fibers within a single Vagus nerve are sensory or afferent fibers. Please don't let my drawing confuse you, they are certainly not arranged like I circled them with blue color. Proportion is my point. These sensory fibers originate in the viscera and end in the Nucleus Solitarius in the brainstem. These fibers are both myelinated and unmyelinated (my sketch says only myelinated, but that's not a fact).
The rest of the fibers within any single Vagus nerve (roughly 20% of them), are the motor or efferent fibers. Most of these originate in the Dorsal (or posterior) Motor Nucleus within the brainstem. These are unmyelinated fibers and they comprise what Dr. Porges named the Dorsal Vagal Complex. His research also point to the fact that this complex of fibers is the most prominent in the sub-diaphragmatic region.
Now, within the motor/efferent fibers we find a subgroup, which is proportionately small - only 15% of the 20% of motor neurons that are actually myelinated! This small portion of the motor fibers originates in a different area of the brainstem - Nucleus Ambiguus - and Dr. Porges names it the Ventral Vagal Complex. This group of neurons primarily innervates the supra diaphragmatic structures.
So easy, right?
Let's take a look at the origin of the Vagus in the brainstem.
THE ORIGIN OF THE VAGUS NERVE(s)

Please note that nuclei are on both sides of the brainstem, it's for the reason of less clutter and overlap that I colored some nuclei on one side, and another on the other side.
It's simple - different origin, different function. Variation in structure (myelination vs. no myelination) affects function as well.
The nuclei which Vagus nerves originate or terminate in are as follows:
Nucleus Ambiguus
Glossopharyngeal nerve (CN IX) and Vagus nerve (CN X) originate from here. This is the origin of the Ventral Vagal Complex.
Fibers originating from here are myelinated, uniquely mammalian, and supply the supra diaphragmatic organs.
Dorsal (or Posterior) Motor Nucleus
This nucleus is the origin of the Vagus nerve exclusively. It is the origin of the Dorsal Vagal Complex, and all the fibers coming from here are unmyelinated. These fibers terminate and regulate sub diaphragmatic organs.
Nucleus of Solitary Tract
Facial (CN VII), Glossopharyngeal (CN IX), and Vagus nerve (CN X) terminate here. NST is a cluster of purely sensory nuclei. It is the first relay station for sensory information incoming to the brain from viscera, face, and special senses (gustatory). NST has a crucial role of integration of the sensory information which expresses in a variety of reflexes controlling breathing, cardiovascular, and gastrointestinal functions.
VAGUS NERVE AND THE SOCIAL ENGAGEMENT

It is in this part of the medulla oblongata in the brainstem that the Social Engagement Magic happens!
So the nuclei that we see pictured in distinct colors in my drawing, are really not as distinct. The medullary nuclei overlap and as they do, they share information. They specifically cross inform with nuclei of cranial nerves V - Trigeminal nerves, VII - Facial, IX - Glossopharyngeal, X - Vagus, and XI - Spinal Accessory nerves.
Autonomic activity can therefore be learned to be read from faces, voices, and postures. If this is new information to you, please refer to Dr. Porges work relating to the Polyvagal Theory.
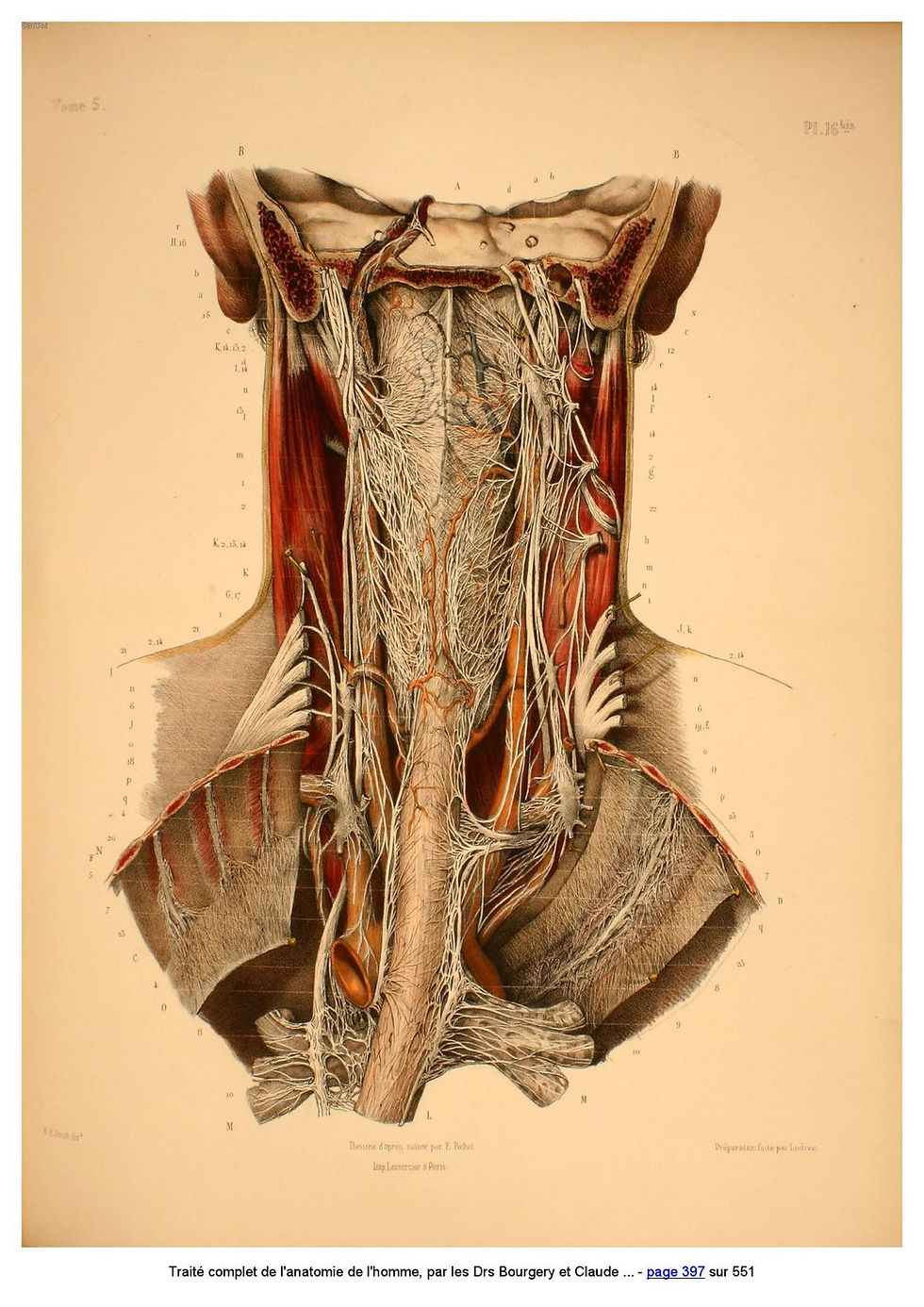
vagal glory in the neck region - Bourgery
WHERE ALL DOES THE VAGUS WANDER?
This nerve covers some serious territory. Anatomy books never show it in its entirety, because it is impossible. But I believe that a good schematic drawing can come pretty close. Take a look at my attempt. I have added my own research to a drawing that I found in Dr. Kuchera's work.
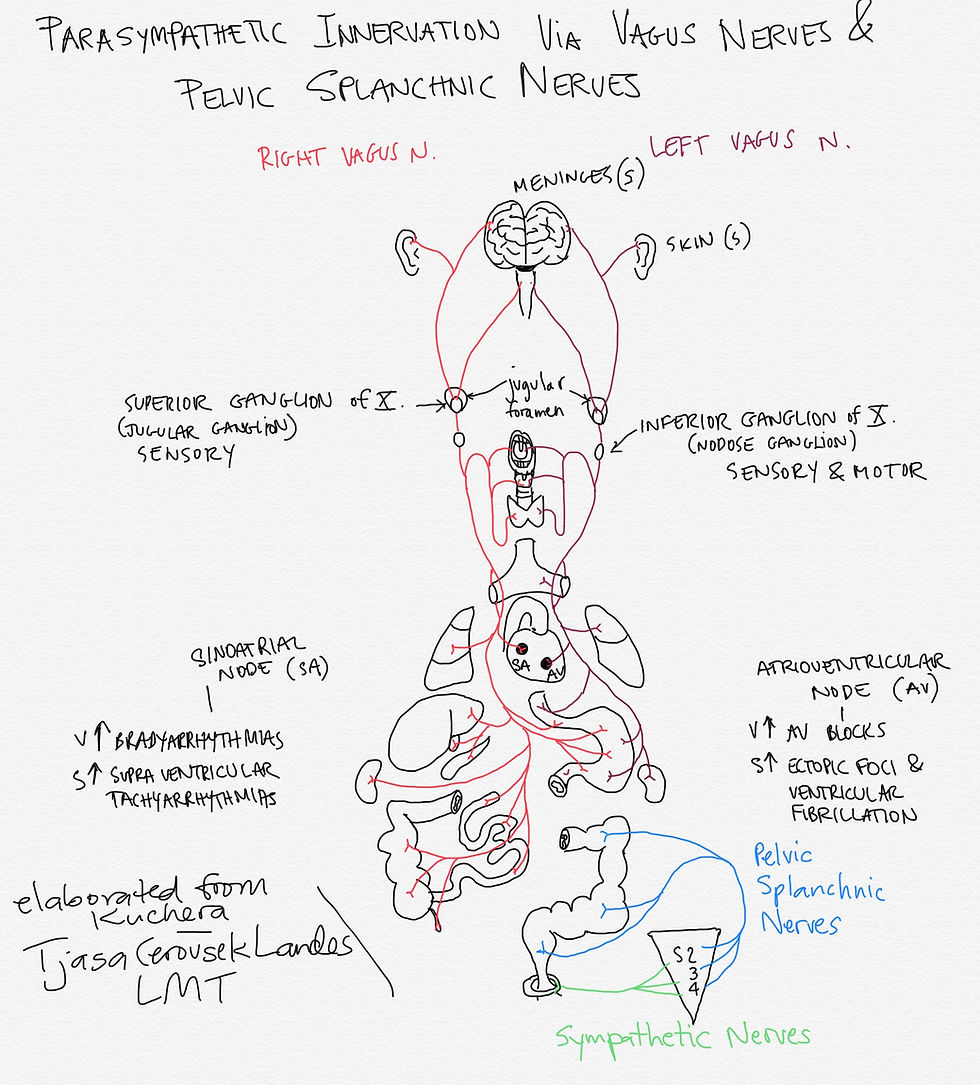
Explanation of the drawing: first of all, there is a tiny portion of sympathetic nerves (in green) reflected in this sketch. Please understand that sympathetic nerves are also incredibly elaborate and they will require their own study and much sketching.
Pelvic Splanchnic nerves (in blue) are not part of Vagus nerve but are parasympathetic nerves as well. Parasympathetic innervation via CN III, VII, and IX is not included in this drawing either.
Vagus nerves originate and terminate in the medullary nuclei (Dorsal Motor, Ambiguus, and Nucleus of Solitary Tract). Left and right vagus nerves (each carrying dorsal and ventral vagal complex) then exit at the jugular foramen bilaterally. Here the Vagus nerves (VNs) exchange fibers with the Superior Ganglion of Vagus aka the Jugular Ganglion. From here, VNs extend sensory branches to the meninges (dura mater) and to the skin of ears.
From the Superior Ganglion VNs fibers continue inferiorly to the Inferior Ganglion of the Vagus aka the Nodose Ganglion. Sensory and motor fibers from here innervate palate, larynx and pharynx, as well as thyroid gland.
VNs continue into thoracic cavity, where left VN rotates to become more anterior, and right VN more posterior. This rotation is caused by embryologic development and rotation of the gut tube, which VNs follows.
The vagus nerve shares sensory innervation territory with the splanchnic nerves (sympathetic nerves). Recent studies demonstrate that the sensory vagal fibers terminate in the muscle layers and their mucosa, whereas the splanchnic sensory fibers predominantly innervate the serous layer (Mei, 1998).
Once within the abdominal cavity, the VNs become known anatomically as the anterior (left) and posterior (right) vagus nerves.
In abdomen, Vagus nerves mingle closely with the sympathetic nerves at prevertebral ganglions and continue alongside sympathetic nerves en route to the organs.
As per Barral, the right Vagus innervates the posterior aspect of Gastro Esophageal Junction and stops at splenic flexure (Cannon-Bohm area). It is the longer of the two Vagal nerves.
The left Vagus nerve innervates the anterior part of the Gastro Esophageal Junction and terminates at the duodenum.
The topic of innervation could consume several pages, but I am going to keep it very short and brief. I hope you enjoyed my very concise offering in the vast knowledge potential of the Vagus nerves and their beautifully complex structure and function.
If you yourself spent many hours studying this subject and believe I have omitted or falsely represented the subject, please let me know and I hope you can share your own research.
I am a student for a lifetime.
Sources & References:
many hours of study with Jean Pierre Barral DO, Alain Croibier DO, and their students
many hours of reading and researching Steven Porge's books and papers
these resources helped a lot, too:
Grant's Anatomy
Netter's Anatomy
Atlas of Surgical Anatomy by JM Bourgery
Osteopathic Considerations in Systemic Dysfunction by Kuchera
Applied Anatomy by Clark

Hi Gabriel,
Thank you for your kind words and yes, I have seen your posters in Facebook Vagus nerve group's post. I can appreciate the time you have invested into the poster production and study that preceded it! Well done and congrats : )
Hi Tjasa- A colleague sent me a link to your page. I love your drawings and explication. In all of the anatomical studies of the vagus I've done, I've found the Bourgery and Jacobs drawings to be the most beautiful. I've been geeking out on this stuff for a decade myself, entering through the doorway of Somatic Experiencing, where I first learned about the theory in 2010. About a year ago we reached out to Dr. Porges and have been working with him for the past 9 months to create a poster of the theory that shows the neuro-anatomy. I thought you might find it useful. It is at https://appliedmindfulness.org/polyvagal-illustrations
Warmly,
Gabriel Kram
Founder, Applied Mindfulness, Inc.
Hello bdiablo,
Well, stomach certainly is connected with the vagus nerve. There are many other connections that could be possibly contributing to headaches in your dad’s case. I will suggest you look up practitioners in your area that can address your dad’s headaches from similar perspective I would. https://www.barralinstitute.com - go to find a therapist and search for practitioners near you that are trained in visceral manipulation (level 5 or higher), neural manipulation (level 5), and craniosacral therapy (level 2). I wish you and your dad the best! If you need more help you can email me directly.
My father suffers from the type of concussion hockey players have, he has had severe headaches daily for 17 years. I have noticed when he eats his headaches worsen...I somehow think his stomach is related to the pain in his head, do you have any information on the correlation between stomach and nerves?
Hello Al - d.alan.theede,
Thank you very much for your kind words. It was indeed a deep anatomical spelunking to pull it all together. But, it's pure joy for me to engage with the material in this way. I'm glad some of you are finding it helpful : )